Introducing Tinea: The Fungal Infection You Need to Know About
Hey guys! Today, I want to discuss a topic that’s been bothering me, and that’s tinea. I’ve seen a lot of people suffering from tinea, and it’s not a fun experience. So, let’s talk about it!
But before we dive into the symptoms and treatments, let’s define what tinea actually is. In simple terms, tinea is a fungal infection that affects your skin. It’s also referred to as ringworm because it often forms a circular rash that looks like a ring.
The thing about tinea is that it can be contagious and spread easily. So, if you suspect you have it, it’s important to get it treated as soon as possible.
Signs and Symptoms of Tinea: How to Recognize This Fungal Infection
Hey there, folks! Let’s talk about the symptoms of tinea. This fungal infection is no picnic, but it’s good to know what to look for so you can catch it early and get it treated ASAP.
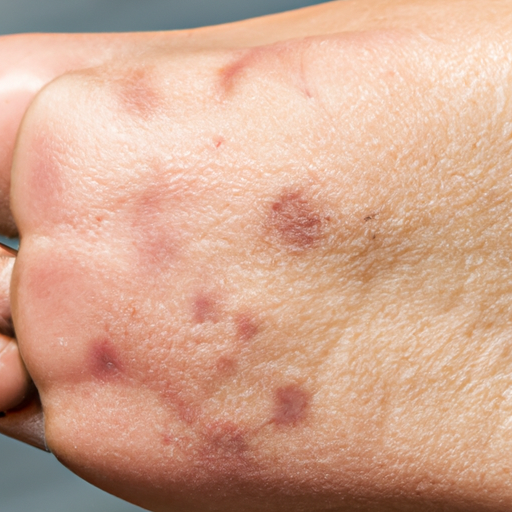
First and foremost, tinea usually shows up as a rash. The rash can be red, scaly, and itchy. It can also be raised slightly off the skin. The rash can show up in different places on your body, depending on the type of tinea you have. For example, tinea corporis (also known as ringworm) often shows up on the torso, limbs or face. Tinea pedis (athlete’s foot) usually shows up on the feet, while tinea cruris (jock itch) shows up in the groin area.
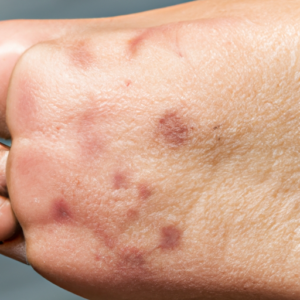
Another symptom to watch out for is blisters. Some types of tinea (like tinea pedis) can cause blisters filled with fluid. These blisters can be painful, but they can also burst and lead to more skin irritation or infections.
If you’re noticing discoloration on your skin, that could also be a sign of tinea. Some people notice that the affected skin is lighter or darker than the surrounding skin. This discoloration can be gradual, so keep an eye out for any changes in your skin’s appearance.
It’s worth noting that tinea can also affect your nails. If you notice that your nails are thick, discolored or brittle, that could be a sign of a fungal nail infection, which is caused by tinea or other fungi.
If you’re experiencing any of these symptoms, it’s important to see a doctor. They can diagnose tinea and recommend the best treatment for your specific case. Don’t try to treat tinea on your own with over-the-counter products, as these can sometimes make the infection worse.
Diagnosing Tinea: It’s Not Always a Simple Process!
When it comes to diagnosing tinea, also known as ringworm, it can be a bit of a tricky process. As someone who has experienced this fungal infection before, I can say that it’s not always easy to identify.
The first step in diagnosing tinea is usually a physical examination by a healthcare provider. They will inspect the affected area, looking for circular or oval-shaped patches with raised edges and clear centers. However, this visual examination is not always enough to make a definitive diagnosis.
In some cases, a skin scraping may be taken from the affected area and examined under a microscope. This can help to confirm the presence of a fungal infection, but it’s also not always foolproof. The results can vary depending on the skill of the technician performing the test and the stage of the infection.
In more complicated cases, lab tests may be required to diagnose tinea. These can include a culture of the skin or a biopsy. These tests can take time and may involve waiting for a few days or weeks for the results to come back.
Overall, diagnosing tinea can be a complicated and frustrating process. It’s important to be patient and to communicate openly with your healthcare provider about your symptoms and concerns. With the right diagnosis and treatment, however, tinea can be effectively managed and eradicated.
Treatment of Tinea
Alright, folks. Let’s get down to business and talk about how to kick Tinea’s butt. After getting diagnosed with Tinea, it’s crucial to begin treatment right away. The treatment options will depend on the type of Tinea infection you have and how severe it is.
To start with, keeping the affected area clean and dry is key to defeating Tinea. Topical antifungal creams and ointments are usually the go-to treatment method for most types of Tinea. It typically takes two to four weeks of using the medication for the rash to disappear fully. Failing to do so could lead to recurring infection, which sucks big time.
In some cases, an oral antifungal medication may be prescribed to get rid of Tinea. Typically, this type of medication is used for severe or persistent infections caused by Tinea. Remember that prescription medications must be taken as directed and for the full course, even if the rash or other symptoms disappear before the medication is finished.
When it comes to treating Tinea on your scalp, medicated shampoos can be an effective way to stop the infection from spreading. Dry your hair thoroughly after using medicated shampoo, and avoid sharing hair brushes, combs, or hats with others. You can also get treatment advice and antifungal products directly from us at BrightSideBeauty.com at our page on treating common types of Tinea.
In summary, treating Tinea involves a combination of keeping the affected area clean and dry as well as using topical or oral antifungal medication. It’s important to start treatment as soon as possible to prevent the infection from spreading and recurring in the future.
So, there you have it, my friends. Now go forth and kick that Tinea’s butt!
Finishing up: My thoughts on Tinea
All in all, tinea can be an annoying and uncomfortable skin condition to deal with, but it is treatable. From personal experience, I know that it can take some time to fully get rid of it, but sticking to a consistent treatment plan is the key.
If you suspect you have tinea, it’s important to see a doctor who can properly diagnose and prescribe the best treatment plan for you. Don’t be ashamed or embarrassed – this condition is more common than you think.
One thing to keep in mind is that tinea can be contagious, so it’s important to take necessary precautions such as avoiding sharing personal items or interacting with others who have tinea if possible. Keeping the affected area clean and dry can also help prevent the spreading and growth of the infection.
Lastly, if you experience persistent or severe symptoms despite treatment, don’t hesitate to follow up with your doctor. They may need to adjust your treatment plan or conduct further testing to ensure proper management of the condition.